Ultrasound scans have become a cornerstone in fertility medicine, offering unparalleled insights into reproductive health. For women evaluating their ovarian reserve, private ultrasound services provide detailed, accessible, and individualized care. This article explores the process, significance, and practicalities of private ultrasound scans for ovarian reserve.
What is Ovarian Reserve?
Ovarian reserve refers to the quantity and quality of a woman’s remaining eggs. It plays a pivotal role in fertility, impacting the likelihood of conception both naturally and through assisted reproductive techniques. Egg quantity decreases naturally with age, with significant declines occurring after the mid-30s. The quality of eggs also diminishes over time, which can increase the risk of chromosomal abnormalities.
A robust understanding of ovarian reserve allows women to make informed decisions about fertility planning, whether for immediate pregnancy goals or future family-building through egg freezing or other interventions.
The Role of Ultrasound in Assessing Ovarian Reserve
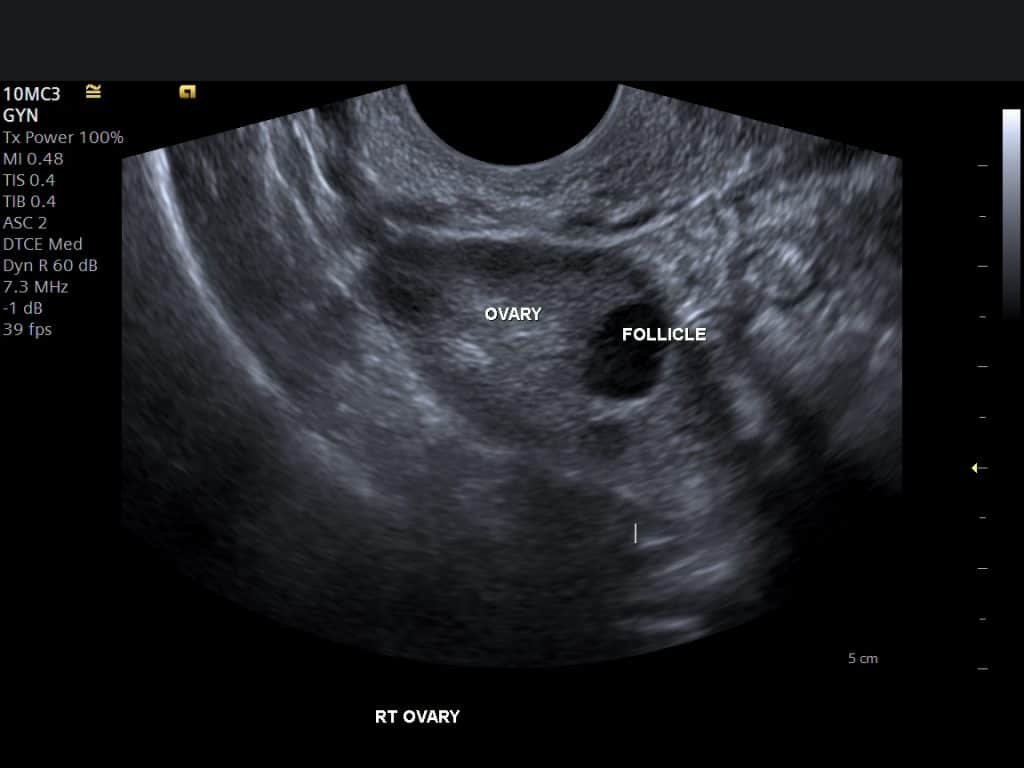
Ultrasound imaging provides an accurate and non-invasive method for assessing ovarian reserve. The key parameter evaluated is the antral follicle count (AFC), which measures the number of small follicles visible on the ovaries during the early phase of a menstrual cycle. Each follicle contains an immature egg, and the AFC serves as a proxy for overall egg reserve.
Compared to other assessments like blood tests for Anti-Müllerian Hormone (AMH) or Follicle-Stimulating Hormone (FSH), ultrasound offers real-time visualization of the ovaries. This allows for the detection of other structural concerns, such as ovarian cysts or abnormalities, that might influence fertility.
What to Expect During a Private Ovarian Reserve Ultrasound
A private ovarian reserve ultrasound is typically performed transvaginally to achieve the highest resolution and detail. The procedure involves inserting a small probe into the vagina, allowing close proximity to the ovaries for optimal imaging. This approach is safe, minimally invasive, and generally well-tolerated.
During the scan, the sonographer measures and counts antral follicles on each ovary. This is done early in the menstrual cycle, usually between days 2 and 5, when follicle visibility is optimal. The process typically takes about 20-30 minutes. Following the scan, detailed explanations of the findings are often provided, helping individuals understand their reproductive potential.
Who Should Consider an Ovarian Reserve Ultrasound?
Private ovarian reserve ultrasounds are beneficial for several groups:
- Women Considering Delayed Childbearing: For those postponing pregnancy due to personal or professional reasons, understanding ovarian reserve can guide future family planning.
- Couples Facing Fertility Challenges: An ovarian reserve assessment is often one of the first steps in diagnosing infertility.
- Women Contemplating Egg Freezing: Accurate reserve data helps determine the feasibility and timeline for egg retrieval procedures.
- Individuals Preparing for IVF: Ovarian reserve directly influences the choice of stimulation protocols and expected outcomes in in-vitro fertilization.
Benefits of Private Ultrasound Services
Private ultrasound services for ovarian reserve offer distinct advantages over standard healthcare routes. These include shorter wait times, flexible scheduling, and personalized care. Private providers often use advanced ultrasound technology for enhanced accuracy and comfort. Additionally, the opportunity for extended consultations ensures that clients leave with a comprehensive understanding of their results.
Understanding Antral Follicle Count and What It Means
Antral follicle count is one of the most reliable indicators of ovarian reserve. Research in the journal Fertility and Sterility highlighted the correlation between AFC and ovarian response during fertility treatments, showing that lower counts often predict reduced success in IVF cycles. Typically, a count of 6-10 follicles per ovary is considered normal, while counts below this range may indicate diminished reserve.
High AFC can suggest polycystic ovary syndrome (PCOS), characterized by excessive follicles that do not mature properly. This condition requires tailored fertility interventions, which can be informed by the ultrasound findings.
The Broader Context of Ovarian Reserve Assessment
While ultrasound provides valuable information, it is often paired with hormonal blood tests for a more complete picture. Studies published in The Lancet emphasize that combining AFC with AMH testing enhances the predictive power of ovarian reserve evaluations. Together, these tools provide insights not only into egg quantity but also reproductive lifespan.
Common Questions About Private Ovarian Reserve Ultrasounds
Private services frequently address practical concerns:
- Cost: Private scans typically range from £100-£300 in the UK, depending on the clinic and included services.
- Safety: Ultrasound is non-ionizing and safe for reproductive health. Transvaginal scans, although intimate, are low-risk and guided by strict hygiene protocols.
- Procedure Length: The actual imaging takes less than 30 minutes, though consultations may extend the appointment.
- Discomfort: While some women report mild pressure during transvaginal scanning, the procedure is not painful.
How Private Services Enhance Fertility Planning
Private clinics often integrate ovarian reserve assessments into broader fertility packages, offering a holistic view of reproductive health. This comprehensive approach supports informed decision-making, whether for timed intercourse, fertility preservation, or advanced reproductive technologies.
Advancing Reproductive Care with Cutting-Edge Ultrasound
Private providers are at the forefront of ultrasound innovation. Many clinics use high-resolution 3D or Doppler ultrasound, which adds layers of detail to ovarian imaging. Doppler can evaluate blood flow to the ovaries, offering insights into ovarian health and function beyond the antral follicle count.
Research from Ultrasound in Medicine and Biology underscores the role of advanced imaging techniques in refining fertility diagnoses. Clinics that adopt these technologies provide a higher standard of care, improving outcomes for clients seeking personalized fertility solutions.
Final Thoughts on Private Ovarian Reserve Ultrasounds
For individuals looking to understand and optimize their reproductive health, private ultrasound services deliver precise, actionable insights. By assessing ovarian reserve through detailed imaging, these scans empower women to take control of their fertility journey with clarity and confidence.