Ultrasound in Pregnancy
Ultrasound is a ubiquitous technology in all areas of medicine but many people are confusing it with other diagnostic imaging modalities. It is not unusual to find people putting it in the same bracket as an x-ray. This misguided impression can quite understandably evoke significant anxiety, especially where pregnancy is concerned.
Let's start by stating a simple but important fact. Ultrasound does not involve ionising radiation.
Ultrasound is a form of sound waves generated at very high frequency. This will be in the range of 3.5 to 7 million cycles per second (Megahertz). Normal sound waves audible to the ear are at a much lower frequency of fewer than 20 thousand cycles per second.
How Ultrasound Works
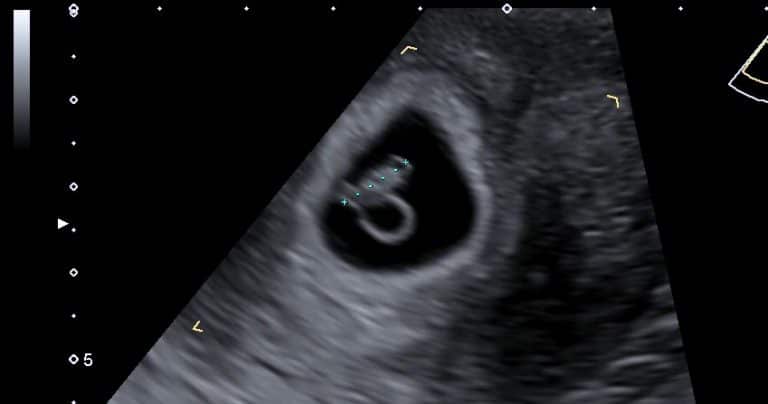
The sound waves are produced by a crystal built in the probe used for the test. The waves are then reflected from the various structures they encounter as they travel through the body. The data produced by the reflected waves is then processed by the computer in the scanning machine to produce an image on the screen representative of the reflecting structures. That is how the detailed image of the pregnant uterus and baby within, complete with movements, is produced and seen in real-time.
The conventional position for an obstetric ultrasound is on your back, usually propped up comfortably to allow you a clear view of the monitor screen. A clear, water-based conducting gel is applied to the abdomen. The gel helps transmit the sound waves. A hand-held probe is then moved over the area in a systematic way.
Alternatively, the ultrasound scan is performed with the probe placed in the vagina (transvaginal ultrasound scanning). This technique often complements conventional transabdominal ultrasound techniques by providing better detail especially in the very early phase of pregnancy such as in the early pregnancy scan. A woman will normally be advised accordingly if this is deemed to be the more appropriate route or sometimes as an additional measure if the abdominal route has not provided all the required information.
Preparation
A full bladder is necessary to get a good picture. Therefore, the person due to being scanned will be asked to drink a few glasses of water (or similar) an hour or so before the test and to refrain from urinating before the procedure. A full bladder is, however, not necessary for the transvaginal Ultrasound.
There may be some slight discomfort from pressure on the full bladder otherwise the procedure is perfectly painless. The conducting gel may feel slightly cold and wet. There is no perception of the sound waves and of-course you cannot hear them.
When to have a Scan
Scans may be performed in the First Trimester to:
- Confirm a normal pregnancy
- Confirm viability
- Assess the baby's age (gestation)
- Assess potential problems such as threatened miscarriage, ectopic pregnancy etc.
- Assess the baby's heartbeat
- Confirm the number of embryos/fetuses
- Identify any abnormalities of the placenta, uterus, and other pelvic structures
- The main early trimester scans are the early pregnancy scan and the dating scan.
In the Second Trimester (after 13 weeks)
- Assess the baby's age, growth, position, and sometimes gender.
- A detailed look at the baby's vital organs and limbs to identify or rule out any possible congenital problems.
- Identify any developmental (growth) problems
- Rule out multiple pregnancies
- Evaluate the placenta, amniotic fluid, and other pelvic organs.
In the Third Trimester (after 26 weeks):
Scans not normally required at this stage except when monitoring pregnancy development and fetal wellbeing in special situations these may include:
- Multiple pregnancies
- Suspected fetal growth problems
- Chronic medical conditions such as diabetes, hypertension, epilepsy etc.
- Pre-eclampsia
Other situations where a scan may be called for are when there is a need to: - Detect cervical changes that might predict preterm labour.
- Verify breech presentation or other uncommon fetal or cord position before delivery.
- Get valuable information leading to treatment of any conditions arising in the course of a pregnancy in a bid to improve a woman's chances of having a healthy baby.
Scan Aided Tests and Procedures
Pregnancy ultrasound plays a crucial role in antenatal care. Some tests which are routinely done for diagnostic purposes are directly ultrasound-guided. Such tests include:
Amniocentesis:
This is the most well-known and commonest invasive test used to make a diagnosis of any condition that may be affecting the fetus. It is commonly performed in the early second trimester (15 – 16 weeks) and is now routinely ultrasound-guided.
An amniocentesis is a test in which the cells that are floating in the fluid surrounding the fetus are examined for the chromosomal pattern of the fetus. The operator will have the ultrasound probe on the abdomen and will guide the fine needle used under direct ultrasound guidance into the womb. Once the tip is seen to be inside a pool of amniotic fluid, a sample will be drawn for the test. Normally this takes a few short minutes and in the vast majority, only one attempt is sufficient.
Amniocentesis results are usually available two to three weeks after the test. Amniocentesis carries a risk of losing the pregnancy of about 0.5 - 1% (1 in 100-200). Age is probably the commonest indication for requesting amniocentesis usually for the diagnosis of Down's Syndrome. This is because, all other factors being normal, the older the mother, the higher the risk of Down's and other chromosomal disorders. A 21-year-old mother has a 1:1700 risk of having a baby with Down's Syndrome, a 30 year old 1:950, at 40 the risk is almost 1:100 and by 45 years of age, it is 1:30.
As mentioned earlier while these statistics refer to the most recognized chromosomal anomaly, there are other anomalies, some of them incompatible with life. It is therefore important for any prospective mother to be aware that the overall risk of all chromosomal anomalies is significantly higher than that of Down's alone at any stage of life. A 201-year-old will, therefore, have an overall chromosomal abnormalities risk (for her baby) of about 1:500 and at 40 the risk would have risen to 1:66.
CVS:
This stands for Chorionic Villus Sampling which simply means taking a biopsy from the developing placenta. It is also ultrasound-guided. The procedure is also performed under direct ultrasound guidance. It differs from amniocentesis in three major aspects:
- It can and is usually performed earlier in the pregnancy. This is towards the end of the first trimester.
- Results are available much more rapidly with a normal turnaround of 48 – 72 hours.
- It has a significantly higher procedure associated miscarriage rate which could be as much as twice that of amniocentesis.
Fetal Echocardiography:
Congenital heart defects occur in about 1% of live births. Causes are multiple and sometimes cannot be identified. Whilst a routine detailed ultrasound scan performed at 18-20 weeks will focus on the heart among other major organs, not all defects will be detected.
It is also sometimes necessary to perform a much more detailed study of the baby's heart. This specialised structural study using ultrasound is called echocardiography or popularly just shortened as ‘echo'. Situations, where this may be recommended, include:
- A family history of congenital heart disease
- An abnormal fetal heart rhythm detected during a routine examination.
- Fetal heart abnormalities detected during a routine pregnancy ultrasound scan
- Abnormality of another major organ system such as the gut or lungs.
- Insulin-dependent (type 1) diabetes
- Exposure to some drugs in very early pregnancy. For example, some anticonvulsants used to treat epilepsy can damage the developing heart.
- If the mother has abused alcohol or drugs during pregnancy
- If a mother has diabetes, phenylketonuria, or a connective tissue disease such as lupus
- If the mother has had rubella during pregnancy
- Diagnosis of some chromosomal abnormalities
Cordocentesis
Sometimes it becomes necessary to obtain a sample of blood from the umbilical cord of the unborn baby, usually for diagnostic purposes. This requires direct ultrasound visualization. This would simply not be feasible without the aid of ultrasound. In some condition, transfusion of blood into the unborn baby is performed. Again, this is directly dependent on ultrasound.
There are many other areas where ultrasound in pregnancy is not only useful but indispensable. These include localization of the placenta which could help determine the safest mode and timing of delivery, checking pattern of blood flow in the cord, a useful feature in monitoring fetal well-being in at-risk fetuses, estimating fetal weight which could be useful in making important decisions and many more.
Biophysical Profile
Sometimes there is concern about the unborn baby's wellbeing. This may be because the baby is not moving well, growth is unsatisfactory or the pregnant mother is suffering from such conditions as pre-eclampsia, diabetes etc. It may, in such circumstances, be deemed necessary to monitor the baby closely and one of the strategies sometimes adopted is to perform what is known as a biophysical profile > With this one checks the baby's movements, general muscle tone, breathing movements and fetal heart pattern. Apart from the latter, the rest is all done by using ultrasound.
Transvaginal Ultrasound scanning
The idea of having the scan performed vaginally can and does provoke anxiety for some women. It is important to say that this is a safe procedure and does not in any way pose a risk to either mother or baby.
In very early pregnancy, this may be the preferable method of scanning as it produces sharper details and may give crucial information otherwise unobtainable (using trans-abdominal scanning).
It is also the case that a transvaginal scan does not require a full bladder, not the most comfortable of requirement especially for an expectant mother struggling with perpetual nausea.
A vaginal scan also circumvents the difficulties with obtaining a good view of the embryo/fetus in early pregnancy for women who are overweight or obese.
Amniotic Fluid
Ultrasound scanning is quite useful in estimating the amniotic fluid volume. This is easy to do and in most cases, this will be normal. However, where the volume is found to be reduced or increased, it could be a very important gauge of the baby's wellbeing. It may also be the first warning that something is not quite right with the baby and could trigger further, more specific, tests.
Serial ultrasound scan monitoring of fluid volume is sometimes used to monitor the progress of a pregnancy and together with other tests could be used to make a decision on the timing and/or mode of delivery.
Placental location
It is not possible through a physical examination to tell the exact location of a placenta in the womb. For the majority of pregnant women, this is really of no importance. However, about 1 in 50 mothers (2%) will have placenta praevia (low-lying placenta) at term. This is a potentially dangerous condition for both mother and baby and most of those affected will need close antenatal observation and delivery by caesarean section. Ultrasound scanning does accurately locate the placenta and aid in making these crucial decisions.
It is important to stress that almost one in five women will be found to have a ‘low-lying' placenta at their 20 weeks pregnancy scan. This is no cause for panic as for the vast majority of them, the placenta will be normally located by the time they get to the third trimester. Many units offer a repeat ultrasound scan at around 32-34 weeks as a form of reassurance.
Placental abruption
Placenta praevia (above) is not to be confused with Placental abruption (abruption placenta). The two conditions are not related even though for both the main concern is severe haemorrhage that is associated with them. In placental abruption, the placenta gets partly or wholly detached from the womb. That will cause bleeding and in most cases, pain. The extent of the bleeding and therefore its effect on the baby will depend on the degree of placental detachment. Ultrasound scanning has a limited role in placental abruption. The diagnosis is mainly secured on a clinical presentation rather than ultrasound findings.
Twins and ultrasound scanning
In days gone by, it was not unusual for twins and rarely other forms of multiple pregnancies not to be discovered until the time of delivery. Ultrasound changed all that. It is exceedingly unusual for that to happen in modern times in most developed countries. Over 95% of mothers in the United Kingdom have antenatal ultrasound scans and the figure is just over 70% in the USA. Even in those countries where ultrasound scans are not offered as a matter of course, the obstetrician or midwife looking after the pregnant woman will suspect the presence of multiple pregnancies in the course of examining her abdomen. This will usually trigger a recommendation for an ultrasound scan. Confirming the number of fetuses is then, in most cases, a straightforward affair.
Identical or not?
Many prospective mothers carrying twins are anxious to know whether the babies are identical or not. In many (but not all) cases it is possible to tell whether they are or not using ultrasound scanning.
If the twins are sharing the same gestation sac or even if they are in different sacs but sharing the same placenta, they are then definitely identical. This is, however, not that common (and a good thing too).
Most twins have separate placentas and sacs. These could be identical or non-identical. It is sometimes possible to tell with a fair degree of confidence whether such twins are identical or not depending on the timing of the ultrasound scan. Of-course if the twins are of different sex, that is confirmatory that they are non-identical. However, it is only possible to tell the gender of a fetus after about 16-17 weeks. The babies have also got to be in a favourable position to be able to do this.
Sharing a sac or placenta not good?
This is not the best form for twins as there are significant potential complications unique to this type of twins. Some of these complications can be life-threatening for the one or both babies. The subject is discussed further in the section on multiple pregnancies.
Doppler Ultrasound
When there are problems or suspected complications, this special type of ultrasound may be employed to try to get important information which may aid in decision making. It takes its name from the 19th-century Austrian physicist Christian Doppler who was the first to describe the phenomenon. So, what is it?
Doppler ultrasound is a form of ultrasound that can detect and measure blood flow. Doppler ultrasound depends on the Doppler effect, a change in the frequency of a wave resulting here from the motion of a reflector, in this case, the red blood cells.
If you are keen to know what the various types of Doppler Ultrasound are, here we will attempt to explain. It is not a walk in the park. Don't say you haven't been warned.
- Colour Doppler -- This technique estimates the average velocity of flow within a vessel by colour coding the information. The direction of blood flow is assigned the colour red or blue, indicating flow toward or away from the ultrasound probe (transducer).
- Pulsed Doppler -- This method allows a sampling volume or "gate" to be positioned in a vessel visualized on the grey-scale image, and displays a graph of the full range of blood velocities within the gate versus time. The amplitude of the signal is approximately proportional to the number of red blood cells and is indicated, not in colour, but simply as a shade of grey.
- Power Doppler -- This device depicts the amplitude, or power, of Doppler signals rather than the frequency shift. This allows detection of a larger range of Doppler shifts and thus better visualisation of small vessels, but at the expense of directional and velocity information.
Color Doppler depicts blood flow in a region and is used as a guide for the placement of the pulsed Doppler gate for more detailed analysis at a particular site.
Doppler ultrasound has many applications including, for example, the detection and measurement of decreased or obstructed blood flow to the legs as in suspected DVT. Colour Doppler ultrasound is done first to evaluate vessels rapidly for abnormalities and to guide placement of the pulsed Doppler to gain sample volume for detailed analysis of velocities.
The bottom line:
It is very difficult to imagine modern obstetrics without ultrasound. It is an integral part of the care of the pregnant mother and her unborn baby and there is no doubt at all that millions of people across the globe arguably owe their lives to this technology which is now taken as a matter of course.
Twins and other forms of multiple pregnancies
Frequency
About 1% of spontaneous conceptions among the Caucasian population will be twins or other less common forms of multiple pregnancies. The rate is slightly higher for those of black African ancestry and somewhat lower for Japanese and others of oriental ancestry. The rate of multiple pregnancies in assisted conception such as IVF is significantly higher.
For any individual woman, family history is a significant factor. If a woman is a twin herself, she has a much higher chance than average of having twins herself. The same applies to a woman who has first-degree twin relatives i.e. siblings or parents.
The rate of identical twins is however constant and is not influenced by age, race, family history or any other factors. Monozygotic twins is another term to describe identical twins. The rate is roughly 4 per 1,000 births.
Twin Issues
Twins may be exciting but these pregnancies also have their own specific challenges. It is important to stress up-front that the majority of twin pregnancies, upwards of 85%, have a completely successful outcome and dispel the impression that twin pregnancy is automatically bad news.
That done, let's turn to the common saying, which happens to be largely true, that doctors and midwives like repeating when speaking about twin pregnancies. The saying goes “all pregnancy complications are commoner in twins apart from prolonged pregnancy”. That is an important and honest starting point. So, when you talk of prematurity, pre-eclampsia, placental abruption, growth restriction, antepartum haemorrhage, postpartum haemorrhage, it is a true general statement that the risk of any of these is higher, the bigger the number of babies a woman is carrying.
Unique Twin Issues:
Increased risk of pregnancy complications is not the only issue that needs to be dealt with. There are problems that are unique to twin pregnancy. The most important one of these is a twin-to-twin transfusion. This condition occurs only in identical (monozygotic twins) and specifically those who share a placenta. The medical term for a common placenta in twins is monochorionic. It is true that twins that share a placenta have got multiple blood vessel communications within that placenta. These communications are not always a problem and in many if not most cases there is no problem as there is physiological equilibration of the blood flow in both. However, for some, these communications are a problem which is sometimes lethal for one or both. This is brought about by an imbalance in the blood flow whereby one ends up as a ‘donor' and the other a ‘recipient'. It means there is a net flow of blood to the recipient and this is the one at greatest risk as he/she gets overloaded.
Can anything be done?
When twin-to-twin transfusion is suspected or diagnosed, the care becomes a specialist issue. There will be serial ultrasound scanning to track the progress of the condition of the twins. Other tests will also be done to keep a close eye on the babies. Sometimes intervention is required to try to reduce the severity of the condition. In most cases, delivery is early to try to prevent further deterioration. Not all cases of twin-to-twin transfusion are that severe. Some are mild enough not to require any intervention.
Vanishing twin
It is true but probably not widely recognised that twin pregnancies in the second and third trimester represent at most two-third of pregnancies that start as such. What does this mean? Basically, it means, a lot more pregnancies start as twins. For a variety of reasons some embryos in twin pregnancies do not make it beyond the first few weeks and these pregnancies continue as singleton pregnancies. Some of these women would have had early ultrasound scans say at 6 or 7 weeks. Presence of twins would have been identified then and a repeat scan a few weeks down the line a repeat scan shows, not two, but one fetus. The other twin has ‘vanished'.
As mentioned earlier, this phenomenon is estimated to affect up to a third of all twins that start as such. Mercifully, this vanishing occurs fairly early before the first scan for most affected mothers and therefore these will be oblivious of the fact that they started off with twins. The loss of the one twin is usually accompanied by very mild or no noticeable symptoms.
References:
NHS - Ultrasound Scan
FDA - Ultrasound Imaging
NHS- Ultrasound Scans in Pregnancy
NHS - 12-week scan
ROOG - Guidance for antenatal screening and ultrasound in pregnancy in the evolving coronavirus pandemic
NICE - Antenatal care for uncomplicated pregnancies
BMUS - Guidelines for the safe use of diagnostic ultrasound equipment
Ultrasound in Obstetrics and Gynaecology - ISUOG Practice Guidelines: performance of first‐trimester fetal ultrasound scan
Healthline - Pregnancy Ultrasound
WHO - WHO recommendation on early ultrasound in pregnancy
Medically Reviewed by Tareq Ismail Pg(Dip), BSc (Hons)